Millions suffer from ‘long COVID’ thanks to micro clots
Thu 6:39 pm +01:00, 31 Mar 2022 2Please send this VERY important “long Covid” article to everyone you know!
Joel S. Hirschhorn trumpets a medical test that can help diagnose patients
By Joel S. Hirschhorn
The Long COVID Alliance says that the chronic condition has impacted 9.4 million Americans … and counting. As shown below many more millions of people are suffering with long COVID and getting little medical help. Long COVID has become its own unique epidemic. This is what a major published medical study in The Lancet had to say:
“Patients with Long COVID report prolonged, multisystem involvement and significant disability. By seven months, many patients have not yet recovered (mainly from systemic and neurological/cognitive symptoms), have not returned to previous levels of work, and continue to experience significant symptom burden.
“The comprehensive assay of symptoms spans 10 organ systems (neuropsychiatric, systemic, reproductive, cardiovascular, musculoskeletal, immunological, head-ear-eye-nose-throat, pulmonary, gastrointestinal, and dermatologic).”
This sounds as bad as the COVID infection pandemic, but it is happening after people recover from the infection, people who had not been hospitalized. Yet they are really suffering.
This is the sad truth. Huge numbers of people who survived initial COVID infection are plagued with many health problems greatly reducing their quality of life. These are now well-known as long COVID victims. Despite lives severely impacted, they have been receiving very little help from the medical establishment. And a major article in The Washington Post documented that working-age long COVID victims unable to work at their jobs have had little success in getting benefits from insurance companies and government agencies. So, in addition to serious health problems many face economic disaster.
The medical issue
A key problem widely known is that physicians have been unable to document through usual testing that long COVID victims have a true medical illness when they complain of multiple serious symptoms. These are salient observations made in the article:
“Patients cite a litany of symptoms that defy verification through basic medical tests. They become exhausted at the merest exertion. They can’t remember simple words. Their hearts feel like they are fluttering. Yet neurological exams, EKGs and chest X-rays come back clean.”
“Doctors said in interviews they are treating long covid patients who are clearly too sick to work but who have difficulty meeting the evidence threshold insurers demand: objective medical test results showing an inability to perform work.”
“The Centers for Disease Control and Prevention acknowledges gaps in medical knowledge regarding long covid. It warns doctors not to rely solely on heart, lung and brain tests to diagnose the syndrome because the symptoms are so difficult to measure.”
“Lack of laboratory or imaging abnormalities does not invalidate the existence, severity, or importance of a patient’s symptoms or conditions,” the CDC cautions in its official guidance.
Wide ignorance of a key medical test
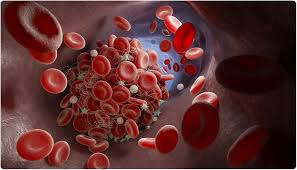
If there is recognition of the proven biological or physiological basis of long COVID, then victims could be given a test used in many circumstances. What research has shown is that long COVID victims have what has been found in many who were infected by the virus or received mRNA COVID vaccines. They likely have micro blood clots throughout their bodies as a result of spike proteins impacting small blood vessels. Micro clots impede oxygen flow to body organs and the brain, with many possible health impacts.
A well-known medical test has been successfully used to determine if there are extensive micro blood clots in a person’s body. It is the D-dimer test. High values prove that extensive clots are present. Yet this medical test seems to be unrecognized by long COVID victims, their physicians and, in some cases, their attorneys. It is essentially “the missing link” in providing victims with medical evidence that their myriad symptoms have a physical explanation.
Relevant medical research
A 2021 medical research article was titled “Impact of persistent D-dimer elevation following recovery from COVID-19.” This is what it dealt with: “One hundred fifty COVID-19 patients were reviewed at St James’s Hospital Dublin between May and September 2020 at a median of 80.5 (range 44-155) days after initial diagnosis. These included patients hospitalized during initial illness (n = 69) and others managed entirely as out-patients (n = 81).” It concluded: “In 15% of the patients recovered from COVID-19, persistent D-dimer elevation was observed after a median of 3 months following COVID-19. These patients had experienced a more severe COVID and still presented more frequently a lower mean [oxygen level].”
Another medical research article titled “Impact of persistent D-dimer elevation following recovery from COVID-19” said: “Increased D-dimer levels (>500 ng/ml) were observed in 25.3% patients up to 4 months post-SARS-CoV-2 infection. On univariate analysis, elevated convalescent D-dimers were more common in COVID-19 patients who had required hospital admission and in patients aged more than 50 years (p < .001). Interestingly, we observed that 29% of patients with elevated convalescent D-dimers had been managed exclusively as out-patients during their illness. In contrast, other coagulation (prothrombin time, activated partial thromboplastin time, fibrinogen, platelet count) and inflammation (C-reactive protein, interleukin-6, and sCD25) markers had returned to normal in >90% of convalescent patients. Elucidating the biological mechanisms responsible for sustained D-dimer increases may be of relevance in long COVID pathogenesis and has implications for clinical management of these patients. ”
It must be emphasized that the D-dimer test has also been used to understand varying levels of COVID illness and death for hospitalized patients. From a study at a major New York hospital system in 2020 these findings show how important D-dimer test data are, and they give the levels of test results that correlate with the worst conditions:
“After controlling for variables as listed above (age, sex, gender etc), it was evident that the magnitude of D-dimer elevation at admission is independently associated with risk of death. Irrespective of age, gender, ethnicity and pre-existing co-morbidity, death was found to be 1.7 times more likely if D-dimer was in the range 0.23-0.50 μg/ml (230-500 ng/ml) at admission, than if it were normal (< 0.23 μg/ml (230 ng/ml)), 2.3 times more likely if D-dimer was in the range 0.5-2.0 μg/ml (500-2000 ng/ml) and 4.2 times more likely if D-dimer was > 2.0 μg/ml (2000 ng/ml).”
“A similar pattern was seen for peak D-dimer levels: magnitude of peak D-dimer (at day 5 of hospital admission) was shown to be independently associated with risk of death. Of those 301 patients with highest peak D dimer (> 10.0 μg/ml (10,000 ng/ml)), 182 (60.5%) had died or been transferred for terminal care at study end. In discussion of their study, the authors summarize the results of other similar studies and briefly review current understanding of the pathophysiology of COVID-19 related coagulopathy and associated D-dimer elevation.”
“This study provides the most robust evidence to date that D-dimer is predictive of serious illness and death due to SARS-CoV-2 infection, and thereby provides further support for the notion that point of care D-dimer testing might be a helpful tool for the early triaging of COVID-19 patients presenting to the hospital emergency department and for monitoring patients during the first week of hospital admission.”
There is great potential that D-dimer test data for long COVID patients could be as significant as for COVID patients, not for correlating with death, but with severity of long COVID conditions. It is plausible to think that those with the highest levels would be suffering with the worst long COVID health problems. Getting effective medical help could be helped by knowing D-dimer test data.
Yale University research found that for long COVID victims, “much of the time extreme fatigue from exercising has to do with the inability of the muscles to take up oxygen from the blood. When cardiopulmonary tests don’t reveal a problem with the heart or lungs, ‘it’s not that they’re making things up,’ said Dr. Inderjit Singh, a pulmonologist at Yale New Haven Hospital. … It may be that the muscles are unable to extract oxygen from the blood.” This finding is consistent with micro clots impeding oxygen flow. Indeed, “There’s some thought COVID can cause some chronic clots or micro-clots in the lungs,” said Dr. Phillip Joseph, also a pulmonologist at Yale New Haven Hospital.
Scope of long COVID problem
A key question is this: How many people are suffering with long COVID? Is long COVID really a major health problem that deserves more serious attention by the medical establishment?
One 2021 study found that more than half of those infected with the virus become long COVID victims. It said: “More than half of the 236 million people who have been diagnosed with COVID-19 worldwide since December 2019 will experience post-COVID symptoms – more commonly known as ‘long COVID’ – up to six months after recovering, according to researchers. The research team said that governments, health care organizations and public health professionals should prepare for the large number of COVID-19 survivors who will need care for a variety of psychological and physical symptoms.”
Another 2021 article titled “Exactly How Many People Have Long Covid?” said: “One report from Imperial College London, called React-2, gives a much higher estimate of the prevalence of long Covid. The study surveyed over 500,000 participants between September 2020 and February 2021, asking them whether they thought they had had Covid-19, whether they had any symptoms from a list of 29, and if so, for how long. It estimated that almost 40 percent of people who definitely had or thought they had Covid-19 still had at least one symptom lasting 12 weeks or more. That’s an estimated 2 million people in England living with the condition between those two dates.”
A recent 2022 article noted: “About 1 in 3 COVID patients have long-haul symptoms after getting COVID-19, even if their initial infection was mild, according to researchers from University of California at Davis. About 100 million Americans ages 18 to 65 have gotten COVID-19 since the pandemic began, according to the U.S. Centers for Disease Control and Prevention. Using the UC Davis figure, that means about 30 million people may have developed long COVID since the pandemic began, with many of them recovering enough to resume work.” But far from all.
New research from Cambridge University found this:
“Around two-thirds of the COVID-19 cohort experienced symptoms of long COVID, defined as a symptom lasting longer than 12 weeks beyond initial date of diagnosis. Among those experiencing long COVID the new research found 78 percent had difficulty concentrating, 69 percent suffered brain fog, 68 percent reported forgetfulness and around 40 percent displayed a condition known as semantic disfluency (saying or typing the wrong word). The study also found those subjects with long COVID experienced significant disruptions to their daily lives. More than half the long COVID cohort were unable to work for extended periods of time and one-third lost their job due to their illness.”
It is important to note that many Americans not in the working class also are victims, including children and the elderly. A study in Israel of children aged 3-18 who had recovered from the virus found that 11.2% reported symptoms of long COVID; that translates to over 20,000 victims.
The recent Washington Post article noted: “In the United States, covid has infected 80 million people and claimed more than 970,000 lives. Doctors have estimated there are 750,000 to 1.3 million or more Americans too sick with long covid to return to their jobs. A recent analysis published by the Brookings Institution, based on data from various studies, suggested that long covid disabilities and workplace absences could account for 15 percent of America’s 10.6 million unfilled jobs.”
Research showed long COVID caused by micro blood clots
In October 2021 the material in this article received considerable attention outside the U.S.
It was titled: “Inflammatory micro clots in blood of individuals suffering from Long COVID.” The research was done at Stellenbosch University in South Africa. Researchers found an overload of various inflammatory molecules, ‘trapped’ inside insoluble microscopic blood clots (micro clots), in the blood of individuals suffering from lingering symptoms experienced by individuals with long COVID.
This important finding was made by professor Resia Pretorius, a researcher in the Department of Physiological Science at Stellenbosch University. She started looking at micro clots and their molecular content in blood samples from individuals with long COVID. The findings have since been peer-reviewed and published in the journal Cardiovascular Diabetology in August 2021.
“We found high levels of various inflammatory molecules trapped in micro clots present in the blood of individuals with Long COVID. Some of the trapped molecules contain clotting proteins such as fibrinogen, as well as alpha(2)-antiplasmin,” Pretorius explained.
This is the first research group to have reported on finding micro clots in the blood samples from individuals with long COVID, using fluorescence microscopy and proteomics analysis, thereby solving yet another puzzle associated with the disease.
“Of particular interest is the simultaneous presence of persistent anomalous micro clots and a pathological fibrinolytic system,” they write in the research paper. “This implies that the plasmin and antiplasmin balance may be central to pathologies in Long COVID, and provides further evidence that COVID-19, and now Long COVID, have significant cardiovascular and clotting pathologies.”
In other words, this research connects with what has been found in COVID patients and users of mRNA COVID vaccines, namely micro blood clots.
At the time of publication they had collected blood from 100 long COVID individuals who participated in the long COVID registry, which launched in May 2021, as well as from 30 healthy individuals.
Conclusions
Millions of long COVID victims would greatly benefit from knowing there is a medical test, D-dimer, that can provide solid medical evidence that their bodies and vascular systems have been corrupted by spike proteins. Micro blood clots confirmed by the D-dimer test can provide proof that their many long COVID symptoms have a biological or physiological basis. When this writer asked physicians what they were doing to treat long COVID, common actions included use of blood thinners and anticoagulants, namely Plavix, Eliquis and aspirin.
Recently, this potential medical solution was cited: “We describe 2 cases of [long COVID] in response to opportune administration of over-the-counter antihistamines, with significant improvement in symptoms and ability to perform activities of daily living.”
What merits investigation is whether people who besides having had virus infection also received mRNA COVID vaccines. The combination could explain extensive micro blood clots and the most severe cases of long COVID because of widespread spike proteins impacting their small blood vessels.
___
https://www.wnd.com/2022/03/millions-suffer-long-covid-thanks-micro-clots/
Please send this VERY important “long Covid” article to everyone you know!











Good article. The knowledge of the D Dimer test will hopefully prove useful to many.
I think there is very little focus on this being a problem for people and since it has been over two years since the initial outbreak I would have expected doctors to know these symptoms and make the above recommendations to patients.