Are COVID-19 Patients in Hospital Really Getting Younger?
Sun 11:31 am +01:00, 17 Jan 2021
Are Covid patients getting younger? The senior doctor who writes regularly for Lockdown Sceptics has taken a look at the data and thinks not.
Recently there have been a series of claims in the media that patients in hospital with COVID-19 are younger than they were in the spring. These assertions have been vigorously contested or supported by contributors to social media, feeding an unhelpful coarsening of debate and distasteful ad hominem attacks.
In my last post I examined one of these claims made by BBC reporter Hugh Pym after a visit to Croydon Hospital. I was unable to find any significant increase in younger patients, either from the latest NHS Hospital data, the ONS death data or the ICNARC ICU audit data to support his assertion.
Having had time to look into the monthly packet from January 14th in more detail, I now examine three other specific claims. Readers may find this information a bit dense and technical, but it’s important to establish whether claims made in the media, which have a substantial impact on public opinion, are backed up by officially published figures. It is only by careful analysis and honest transparent discussion that we can arrive at the truth. No one is infallible, which is why peer review is important.
The usual caveats apply: We can only assess the information the NHS allows us to see in the form in which they present it (which leaves a lot to be desired) – and we have to assume it is accurate.
- On December 31st, a nurse at King’s College Hospital gave an interview to Adrian Chiles on Radio 5 live in which she said there were many more children affected by COVID-19 in the winter compared to the spring. She said there was a “whole ward” of sick children in her hospital and many of her colleagues in other trusts had the same problem.
- An ICU consultant at Queen Mary University, London has said there are more younger people in ICU with COVID-19 compared to the spring.
- In an interview on Sky TV, a doctor from the Royal Surrey county hospital said that the patients with COVID-19 were sicker and younger in the winter than in the spring.
I have examined the available data to see what quantitative evidence from the official figures there is to support these assertions.
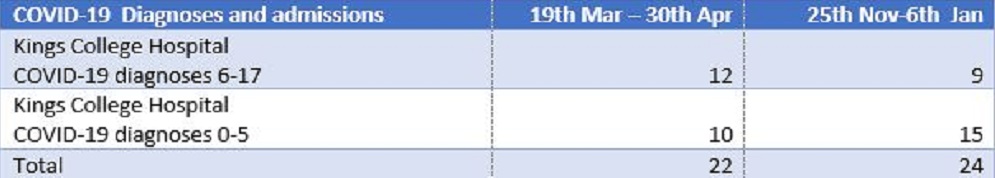
Table 1 shows the total number of COVID-19 diagnoses made on children at Kings College Hospital in two comparable six week periods from the spring and the winter. There is no significant difference between the two periods. Twenty four patients admitted over six weeks with short lengths of stay does not constitute a “ward full” of patients.

Graph 1 shows the number of COVID-19 inpatients at two leading children’s hospitals. Great Ormond St in London and Alder Hey in Liverpool. The graph shows that there are fewer children in both hospitals in the winter than in the spring. The overall numbers are low, fewer than 30 at the spring peak, fewer than 20 in the winter. Great Ormond Street in particular has seen very low numbers of children ill enough with COVID-19 to warrant admission this winter.
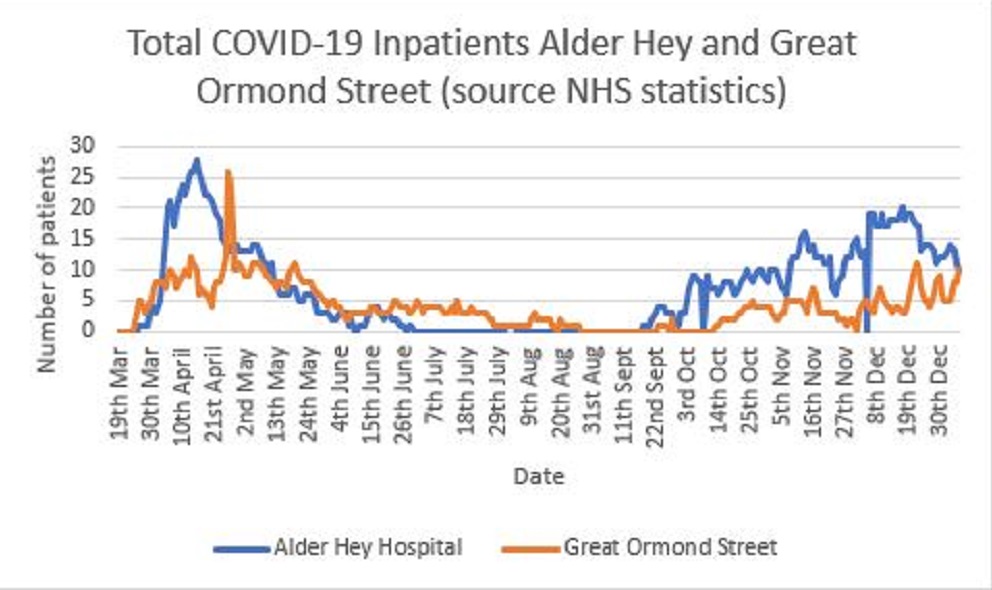
So, I don’t think the data published by the NHS supports the assertion that there is an increased proportion of children sick with COVID-19 compared to the spring. This begs the question, why did the nurse make such a statement, and does she have convincing evidence to back it up which contradicts the officially published figures?
I did notice that the teaching unions retweeted the interview immediately after it was broadcast. It was around the time when they were agitating for the Government to close schools. Correlation does not imply causation of course, but it does seem a curious temporal juxtaposition.
ICU COVID-19 Age Profiles
Table 2 shows age stratification data from 14,710 patients admitted to ICU in England between Sept 1st and January 14th published in the most recent ICNARC audit. It shows that 8.2% of admissions to ICU in the period were under 40. That doesn’t seem to be an excessive proportion of younger people.
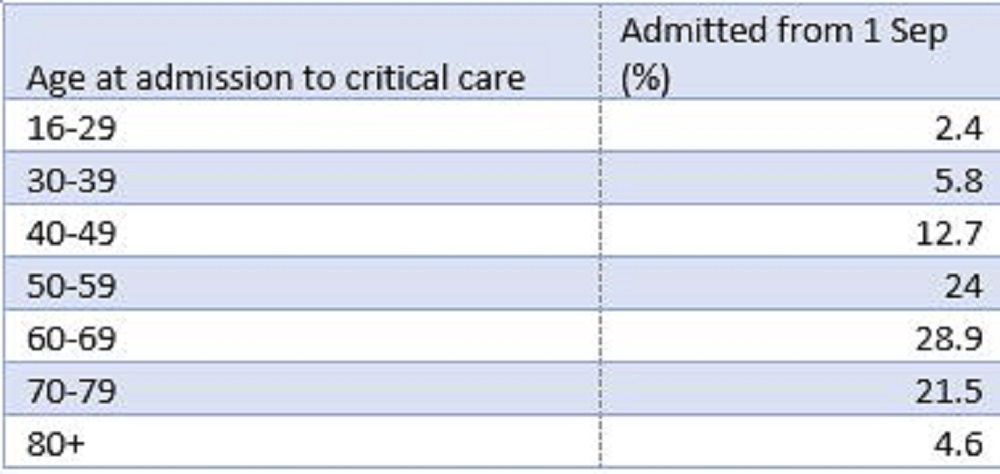
Unfortunately, the raw data for the period up to August 31st is not available on the ICNARC site. However, the same information was used in a recently published paper in Intensive Care Medicine called “COVID-19 in critical care: epidemiology of the first epidemic wave across England, Wales and Northern Ireland”.
In the paper the age groupings were quoted slightly differently to the raw data from the cohort of patients from September to January, so I have aligned the information enabling a direct comparison between the ages of ICU patients in the spring and the winter in Table 3. The only difference is a skew to the older age group in the winter. The data reported in the literature from ICUs in other European countries are broadly comparable with the UK ICNARC figures.
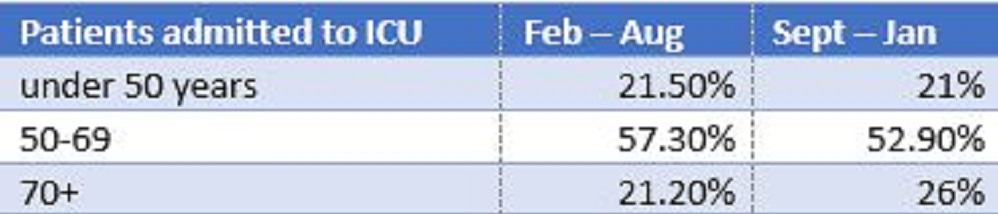
I have not been able to find detailed information as to the age profile of patients in ICU at Barts and the Royal London to compare with the national figures, so it is entirely possible that their local population differs significantly from the national case mix. On a national level there appears to be no significant difference between the age profiles of ICU patients between spring and winter in the figures I have access to.
Searching the published literature on PubMed I can find a couple of relevant papers. Johns Hopkins University in Baltimore noted in the Lancet in April that clinical obesity was associated with younger patients being admitted to ICU.
Another study looked at increasing proportions of younger American patients testing positive for COVID-19 in the community and concluded this was a consequence of increased testing rather than a change in the demographics of the disease.
I wondered whether there might be a difference between age mixes in London compared to the whole of England. Table 4 suggests not. There is a slight skew towards the middle 18-64 band in London compared with the national figures, but London figures comparing spring to winter show the same percentages within each age band; nothing to indicate a major shift to younger people. Readers should note that the lower total numbers of patients in the spring is probably a testing artefact; much more testing is being done now than earlier in 2020, but the age stratified percentages are remarkably stable.
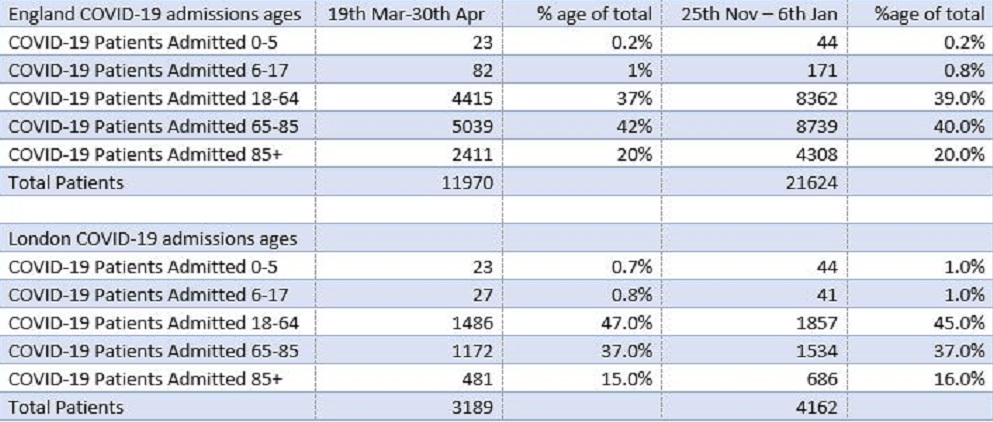
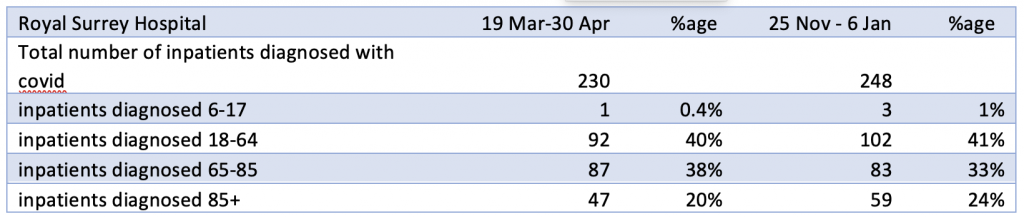
Table 5 is a comparison of the age stratified COVID-19 diagnoses at the Royal Surrey Hospital between comparable six week periods in the spring and winter. The data is contained in the monthly summary of NHS COVID-19 activity published on January 14th. The figures show a slight increase in the percentage of patients over 85 years in the winter compared to the spring. There is no significant increase in patients in the younger cohort 18-64. Unfortunately, the NHS figures do not allow a more detailed analysis of this wide age band, so it is possible that within the 18-64 cohort, the numbers could be skewed to the younger side. Publication of local audit figures would be informative.
The NHS could also be more helpful in their presentation of the numbers. Simon Stevens reportedly told MP’s last week that under 55 year-olds made up 25% of hospital admissions.
That is consistent with the data presented in the 18-64 age group discussed above. He did not comment on whether the proportion of younger patients had changed since the spring. The NHS clearly has the granular figures on age stratification; it would be useful if they could present the data more precisely so the public had accurate figures to compare against media reporting.
Why does any of this matter? If there are a larger number of younger patients in hospital with COVID-19, does that really make any difference, as long as the mortality rate remains low?
From the broader medical perspective it probably doesn’t matter at all, unless there is a significant change in the way younger people need to be managed to achieve better outcomes. If there is new clinical information relevant to treatment, that needs to be disseminated rapidly in the online medical press. I can’t find any such reports in the medical literature over the last two months in relation to younger age groups being affected more by COVID-19 in the winter compared to the spring.
On the other hand, doctors making claims in the media about COVID-19 which cannot be supported by published evidence does matter. In the current febrile climate, where alarmist reporting generates excessive public anxiety and increased social antagonism, it is important that medical professionals are careful only to report matters in the media that can be substantiated – and the plural of anecdote is not data.
Reporting that COVID-19 patients are younger and sicker than in the spring implies that the ‘new variant’ attacks younger people more readily than the previous manifestation of the virus and this clearly generates alarm in the population at large.
If doctors have evidence that COVID-19 is affecting a disproportionate number of young people, then that evidence should be published in the peer reviewed journals via online portals so the whole profession can have a look at it – not issued as ad hoc sound bites to reporters panting for a sensational story or as Twitter clickbait. If the publicly available information does not support the assertion, the suspicion will be that the thrill of being in the media spotlight has got the better of sound clinical judgement.
https://lockdownsceptics.org/










