Is the NHS in Danger of Being Overwhelmed?
Tue 9:58 am +01:00, 27 Oct 2020
Just how great a risk is there of the NHS being overwhelmed? We’re constantly being told by Boris Johnson, Matt Hancock and others that unless we observe the traffic light restrictions in our area, we will witness the kind of scenes we saw in Lombardy back in March, with Covid patients dying in hospital corridors. But is that true? Not according to my friend who’s worked as an NHS doctor for the past 30 years. Here is his guest post for today’s Lockdown Sceptics.
The last three weeks have seen much speculation about the numbers of COVID patients in intensive care units, particularly in the North West and London. Further local lockdowns have been enforced by the Government in the North West, London and yesterday in the Midlands on the grounds that the NHS risks being overwhelmed. But how close is the system to being swamped, and what can we reasonably conclude from publicly available information?
NHS data released to the public to date is incomplete and usually a week in arrears. Carl Heneghan and Tom Jefferson point out in their recent Spectator article that this crisis has been characterised by sequential data inadequacy from the Government’s scientific advisors, Public Health England and the NHS. As they say “a look back at the figures issued shows that the track record, eventually validated against the facts, is abysmal. This is important because major decisions continue to be taken on the strength of such data”.
Some of these mistakes relate to crass errors of basic management, others more disturbing over-exaggeration or over-extrapolation of the size of the threats to public health. It is known that more granular data exist – for instance around the cause of death statistics and in-hospital Covid infection rates. But these figures are not being released to the public by the NHS despite requests for more transparency – seemingly at odds with Freedom of Information obligations.
The data we do have throw up some interesting patterns.
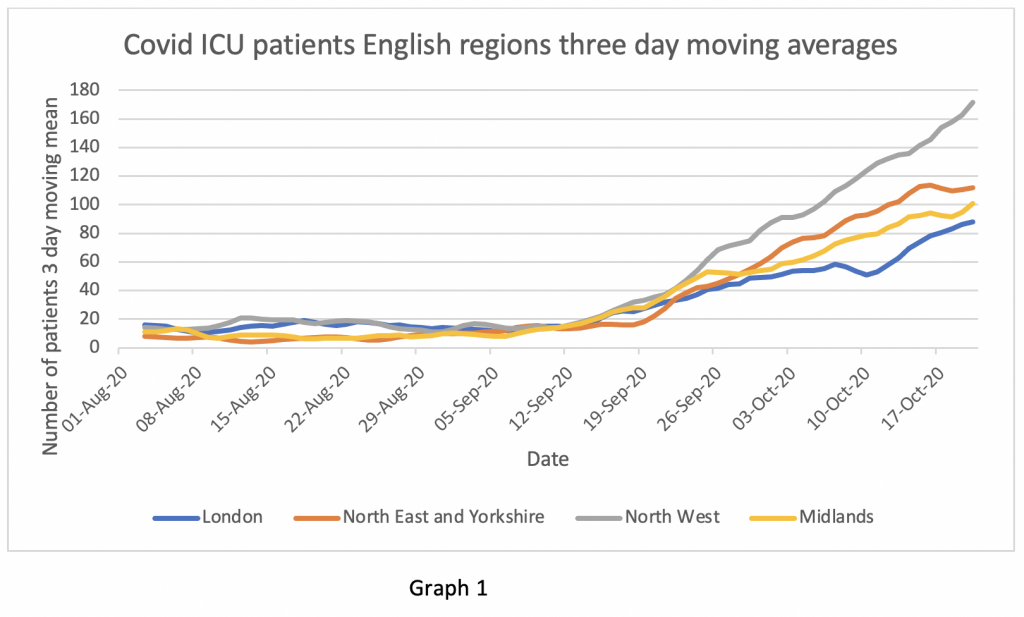
Firstly, the rate of change of numbers of patients in ICU appears to be levelling off in all regions other than the North West up to October 20th (Graph 1). What happened after that we are not permitted to know.
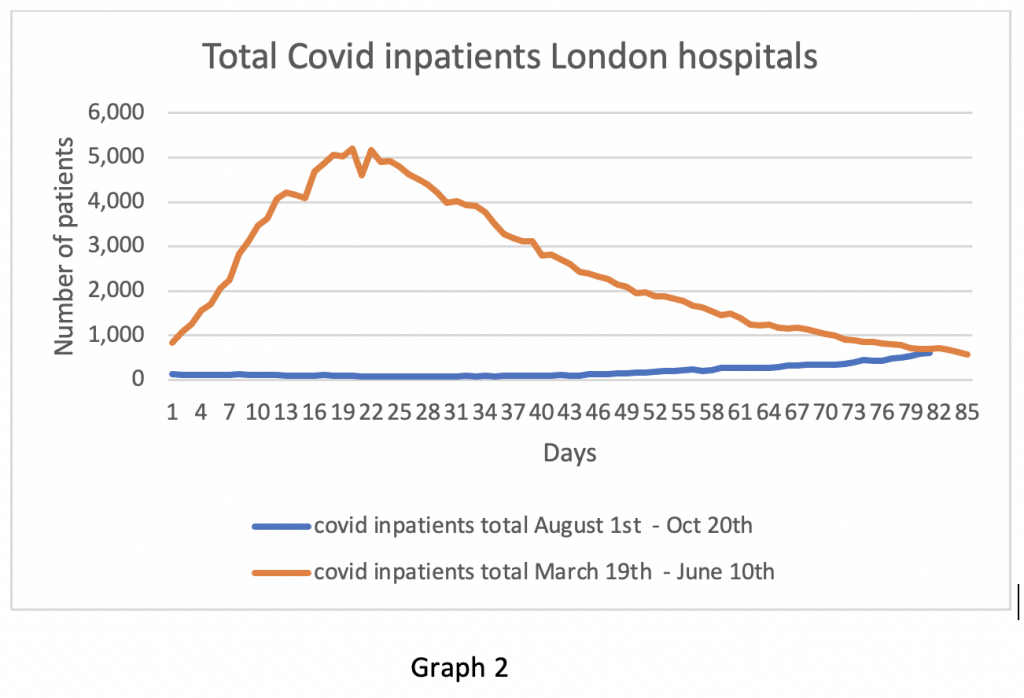
In comparison with the spring surge of Covid, the curves seem very different, especially in London (Graphs 2 and 3). It is clear that the rate of increase in the autumn is nowhere near as steep as in the spring. Further, the number of patients in London ICU beds is not out of proportion to what one would generally expect from respiratory infections at this time of year.
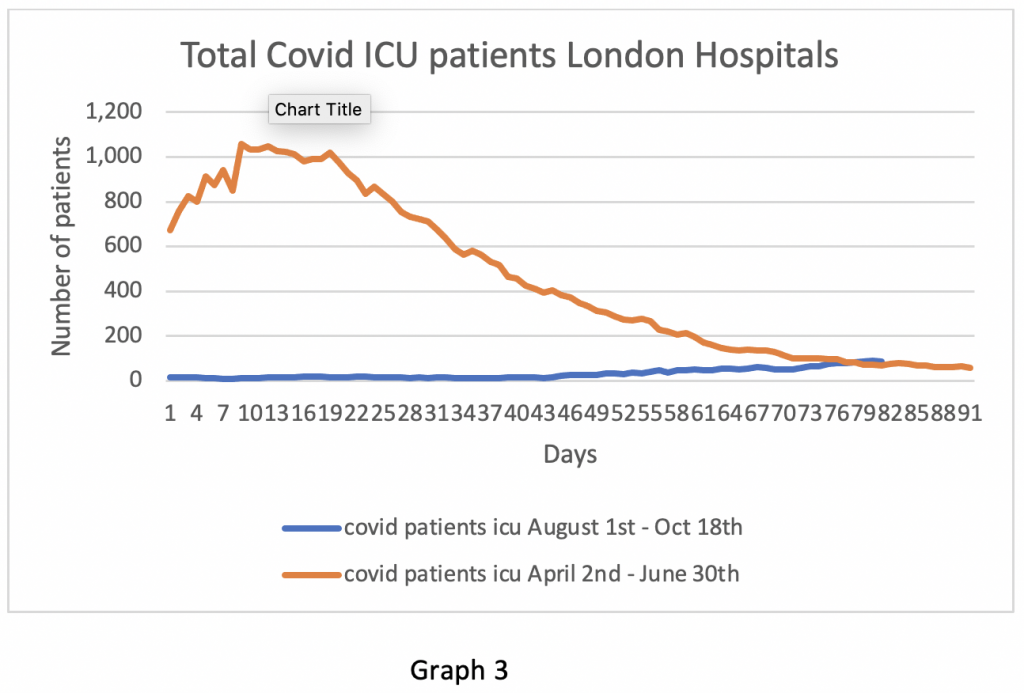
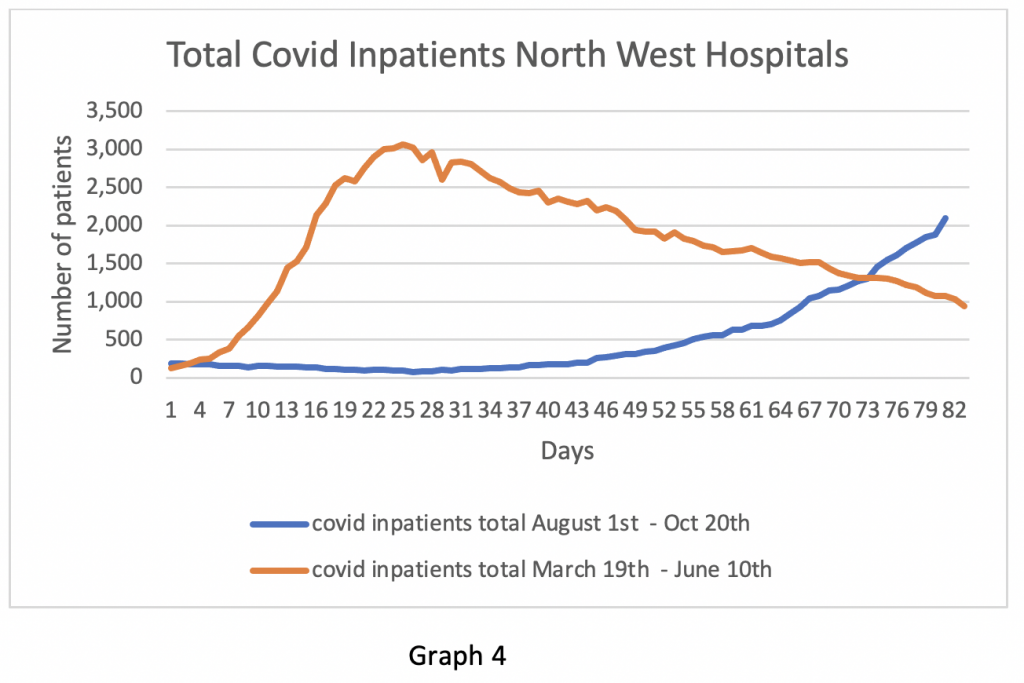
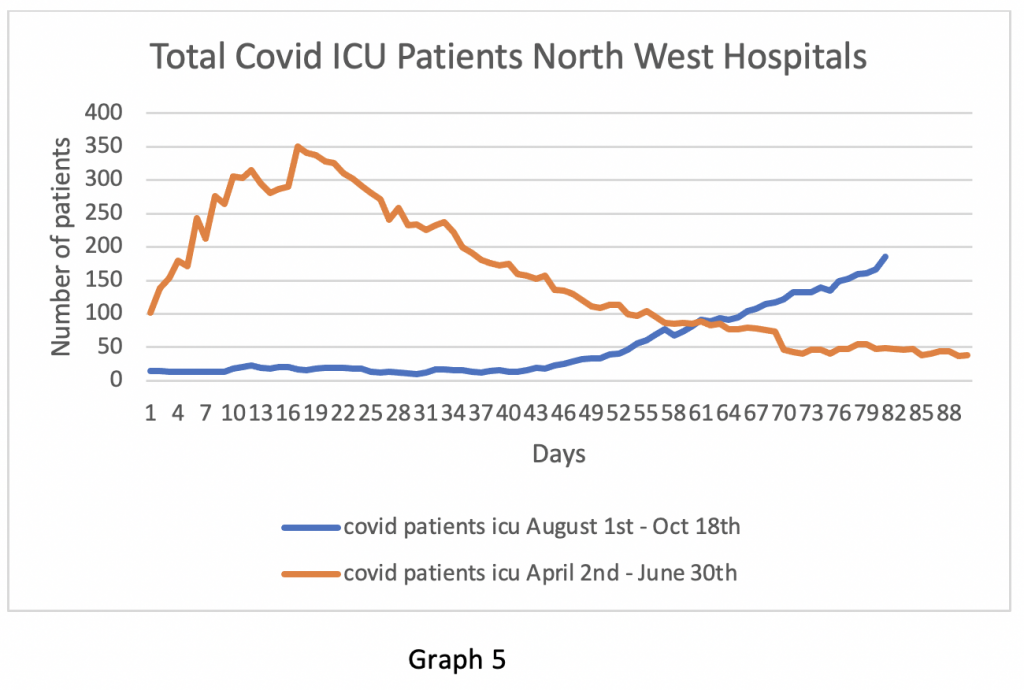
The data curves from the North West look different to London (Graphs 4 and 5). Again, the ICU patients track the ward inpatients, but the slope of the graphs is steeper in the autumn. Why the difference? Broadly, there are two schools of thought. The first maintains that the London population has a higher immunity or resistance to COVID-19 after having been hit harder in the spring. The North West had a surge in the spring too, but national lockdown occurred before the Northern surge was fully mature, hence there may currently be more susceptible people in the North West for the virus to infect than there are in London. Serology data on antibody levels suggests that London has a significantly higher proportion of people with antibodies than the rest of the UK (approx. 15 – 20%). It is reasonable to assume that London also has a higher level of people with T-cell immunity on the basis of greater previous viral exposure.
The other school of thought holds that there is no difference in the resistance profiles between the London and North Western populations, and that the difference in hospitalisation rates is due to poor social distancing habits in the North West and more working from home in the London population. This view inclines to the belief that eventually the ‘second wave’ will travel from the North to London with a lag time of about two weeks.
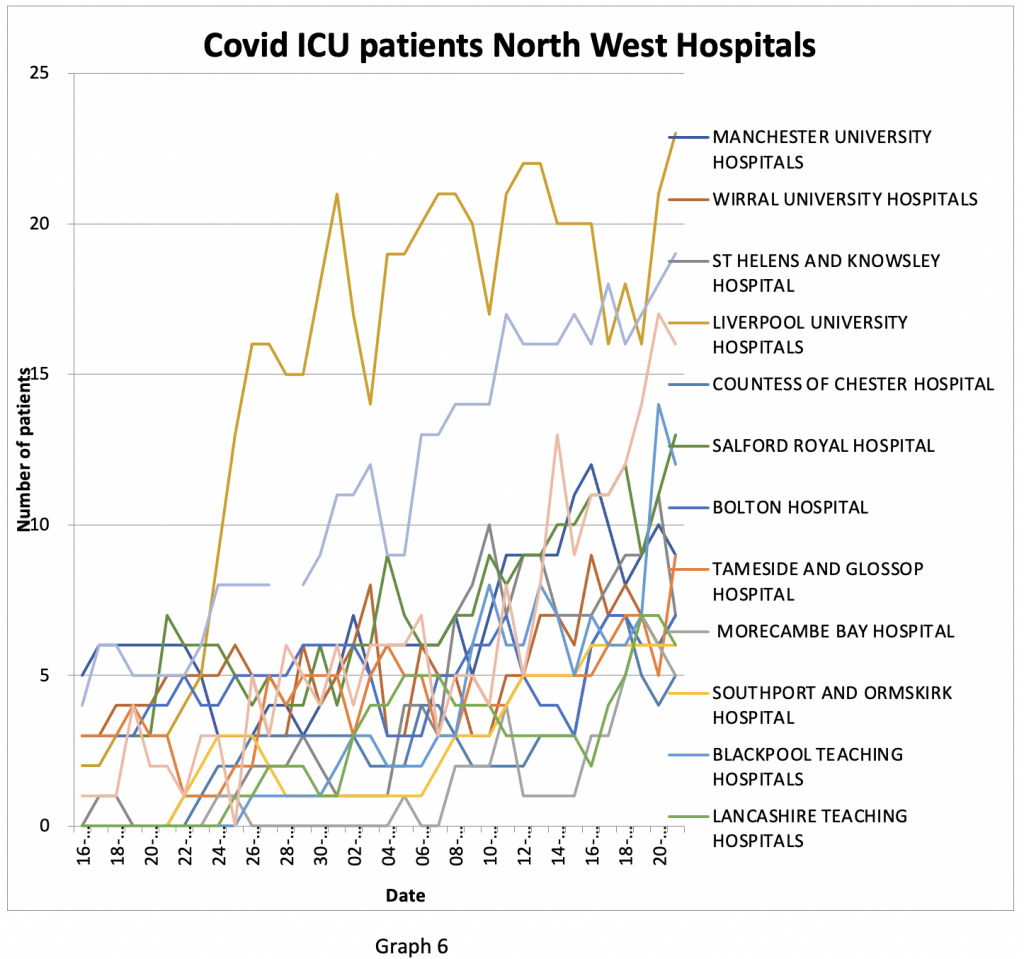
A deeper analysis of the data suggests this is unlikely to be the case. There is a clear inflection point in the North West where ICU cases of Covid start to rise on or around September 22nd (Graph 6). ICU data by individual hospital can be difficult to interpret as intensive care units usually operate as a network involving several hospitals. In a surge crisis, the larger inner-city hospitals usually receive patients from smaller peripheral units, increasing their apparent numbers accordingly. In the North West, almost all the hospitals saw a sudden increase in ICU cases after September 22nd.
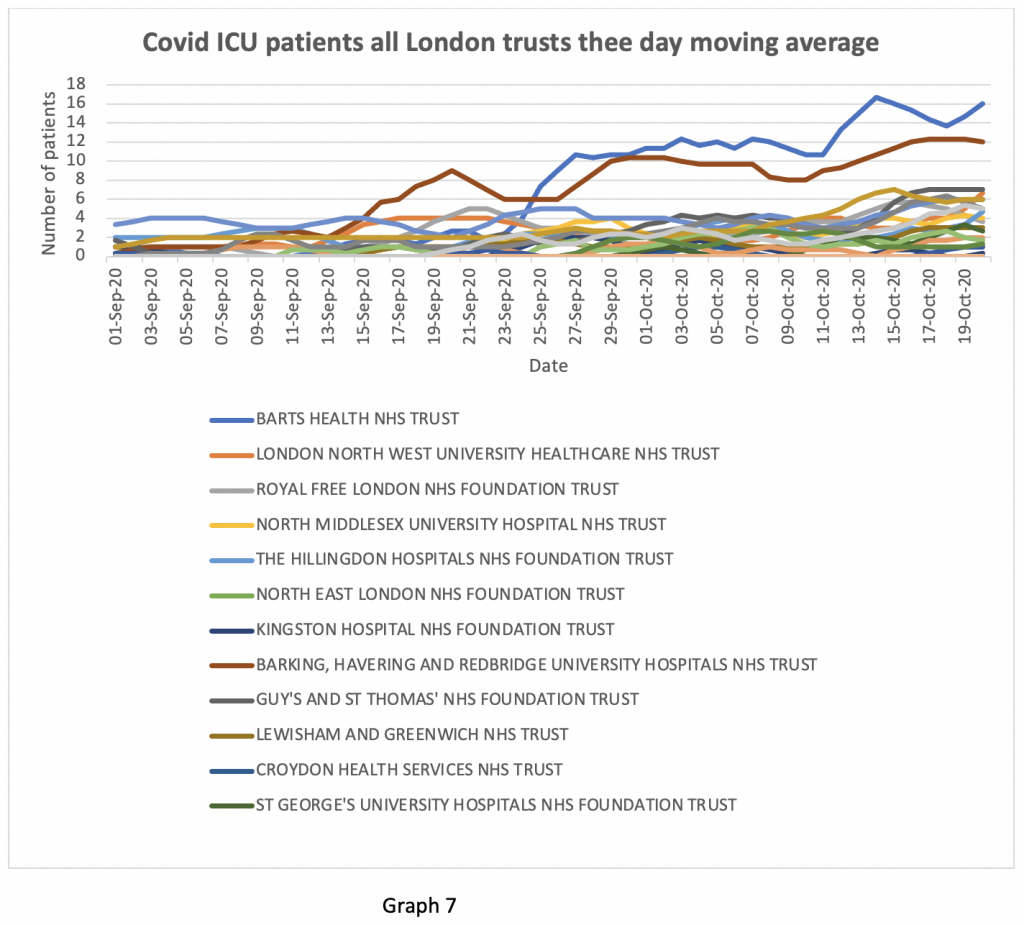
The inflection point in the London figures is different and the distribution of cases between trusts is also very different (Graph 7). Overall numbers are substantially lower than in the North West – a region of roughly comparable population. In London, ICU cases started to rise on September 20th – so, rather than being two weeks behind the North West, London may be seeing a ‘second wave’ at roughly the same time. Unlike the North West, where cases were spread equally between hospitals, cases in London were concentrated in the East of the City, with Barking and St Barts seeing the majority of cases. Hospitals which had been seriously stretched in April, such as Lewisham, Guys and St Thomas’s, the Whittington, St Georges and Northwick Park, have so far not seen many Covid patients, lending support to the enhanced resistance theory.
So what does all this mean? The fact that respiratory infections increase in autumn is not a surprise – the annual winter beds crisis has been a constant feature of my three decades in medicine and cancellation of routine surgical work due to winter pressures is commonplace. Certainly, it is very difficult at the moment for hospital staff in the North West – having been in the eye of the storm last time round, I have the utmost sympathy for them. However, the Mayor of Manchester and the head of the regional ICU network in the North West have both stated on the record that the healthcare system can cope with the surge. Meanwhile in London, Covid patients occupy 10% of ICU beds – completely in line with normal winter pressures at this time of year.
An objective reading of the available data does not currently support the hypothesis that the NHS is in imminent danger of being over-run. The argument from ‘circuit breaker’ advocates is that winter pressures may increase in the coming weeks and create further stress on the system – and that may come to pass, but should Covid admissions or influenza cases increase, there are several measures hospitals can take to manage the problem, such as cancellation of elective work, and use of overspill facilities constructed in haste and at substantial expense in the spring, before resorting to mass incarceration of the public and destruction of viable businesses.
So why the Tier 3 lockdowns in the North and now the Midlands?
Governmental restrictions of civil liberties must be a last resort in a democratic society. To justify such radical measures, both the Government, their scientific advisors and the NHS must be more honest and transparent with the public in respect of the data driving lockdown decisions. Simply asking the population to trust the experts is insufficient, particularly when the experts have clearly been so seriously in error in recent months.
Failure to provide sufficient evidence to justify unprecedented curbs on citizen’s rights suggests arbitrary deprivations of civil liberty are being enforced for political reasons rather than medical necessity.
Trust and confidence are essential for the operation of a modern liberal democracy. Our current leadership is rapidly running out of both.
By
https://lockdownsceptics.org/










