PCR Test
Wed 4:02 pm +01:00, 5 Aug 2020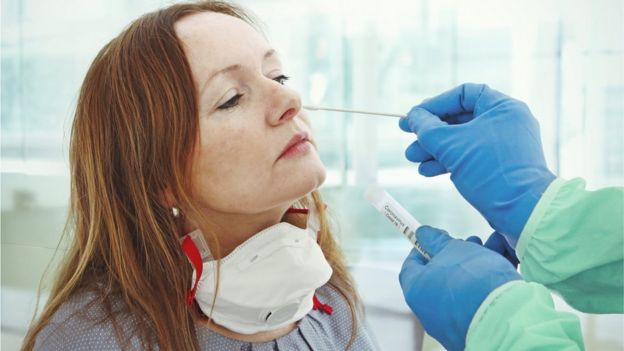
A reader with a background in infectious diseases has emailed me in answer to the question I posed yesterday about the reliability of the PCR test. This won’t surprise anyone.
Your reader’s comments on the PCR test are interesting. It’s worth noting that the test have been in existence for decades but has never been fully tested for efficacy. The manual issued by the Center for Disease Control (CDC) in the US actually states the following at the very start of the document: “Results are for the identification of 2019-nCoV RNA. The 2019-nCoV RNA is generally detectable in upper and lower respiratory specimens during infection. Positive results are indicative of active infection with 2019-nCoV but do not rule out bacterial infection or co-infection with other viruses. The agent detected may not be the definite cause of disease. Laboratories within the United States and its territories are required to report all positive results to the appropriate public health authorities.”
So it was acknowledged not to be virus-specific reliable but nevertheless made positive PCR results notifiable. Brilliant stroke.
Meanwhile, the reader who posed the original question has followed up with a few more:
There are two other aspects of Government testing I find confusing and misleading
When working with biological and biochemical test data, it is important to understand what the test is measuring. There is a general perception, endorsed by the media and Government spokespeople, that the RT-PCR test detects the presence of the virus in swabs. It does no such thing. It detects a segment of one component of the virus, namely the RNA molecule contained within the virus capsule. The segment detected could have arisen from an intact viable virus particle, from a non-viable virus particle or from residual material or debris from virus particles destroyed or degraded by the host’s immune response.
Where the donor has symptoms and their swabs produce a positive result it is reasonable to conclude that they are probably infected with the virus. On the other hand, where the donor experiences no symptoms at the time of sampling nor within the next few days, most likely a positive test result would be derived from debris of degraded virus particles, in which case the donor would neither be infected nor infectious. This latter point neatly explains how donors can test positive but be asymptomatic: they would have been infected in the days before testing with symptoms unnoticed or inconsequential and which infection their immune system effectively fought off.
Of course, all testing to date assumes that we know what the pathogen causing COVID-19 is. Many years ago, Koch proposed criteria for establishing the causative agent of infectious diseases and these have been adapted to encompass viral diseases. Essentially, they require that the virus be isolated and purified, that it is shown to replicate in relevant host cells and that it demonstrates the symptoms of the disease when dosed to an appropriate animal. In January, RNA from a supposed virus was sequenced, shown to be related to the Sars virus and named SARS-CoV-2. Perhaps your readers may know to what extent the criteria have established that SARS-Cov-2 is the causative pathogen of COVID-19. In particular, I am not aware that any virus has been shown to induce the same symptoms and disease progression in animals.
Back in December and January, when COVID-19 was new and spreading rapidly, assumptions had to be made and shortcuts taken. There was no time to do the basic studies in logical order. We are now 8-9 months into the disease and there has been time to do these studies. Until they are done, we have to take it on faith we are testing for the right causative agent.
By / 5 August 2020
https://lockdownsceptics.org/










